By: Dr. Stephanie Duffey • May 19, 2020

By: Dr. Stephanie Duffey • May 19, 2020

Stephanie Duffey • Jul 06, 2020

By: Dr. Stephanie Duffey • Feb 17, 2020
By: Dr. Stephanie Duffey • Dec 04, 2019
As a physical therapist, I’m often asked the question, “How do I know when I need to slow down, stop, or keep going?” It’s a valid question, and one that many people struggle to identify. It’s challenging to interpret what you’re feeling in your body, when you can push harder, and when you need to scale back. So, to keep things simple, I came up with a little something I like to call the stoplight method. Let’s break it down.
Green Light: When you’re operating at the green light level, you’re able to exercise with no aches and pains and you may even be looking for ways to intensify your workouts. If you’re a runner, you’d be able to maintain the current pace or distance that you’re following with no discomfort. This is where you want to be (but I know this isn’t always possible or realistic).
What to do: Maintain what you’re doing, or experiment with advancing to the next level. For runners, this means working toward a faster pace or increasing your mileage.
Yellow Light: Signs to look for if you’re approaching the yellow light include light soreness or achiness that persists for more than 24 hours after your run, a small limp when running (but not when walking), and slight swelling of your joints after a run.
What to do: Slow down a bit—this is your body telling you to back-off. Take a rest day and re-evaluate how you’re feeling. Try to recognize patterns. For example, maybe your knees start to hurt when it’s time to get new running shoes, so take a trip to the shoe store! Listen to your body and take action if there’s a behavior you need to change to feel better and enhance your performance.
Red Light: If you’re approaching the red light, you’re experiencing very sharp pain that stops you in your tracks. The pain is debilitating and you are unable to walk without a limp. You may be experiencing intense swelling in your joints and intense discomfort that doesn’t subside after 24 hours.
What to do: It’s time to consult an expert. You may be at risk of a stress fracture or other serious injury. While it’s challenging to seek help and cease physical activity, it’s important to be seen by an expert early, so your injury doesn’t intensify. You may also be able to recover more quickly if you get help for the problem earlier rather than later.
I hope my simple stoplight method helps you identify how to deal with the pain you may be experiencing in your body and the action steps you need to take to feel better.
Need help from an expert? Let’s chat!
By: Dr. Stephanie Duffey • Mar 02, 2020
Other than identifying what caused the irritation in the first place, here are some of my other tips for managing plantar fasciitis:
By: Dr. Stephanie Duffey • Apr 21, 2020
Paul Linden, PhD
PaulLinden@aol.com • www.being-in-movement.com
Love without power is ineffective.
Power without love is brutality.
Conflict is commonly approached as mental, emotional, spiritual, political, cultural and historical in nature. However, the body’s responses are crucial and are often ignored. Self-regulation on the body level must be a part of the peace process.
The five exercises detailed below are based on my 49 years of practice of Aikido (a nonviolent Japanese martial art) and body awareness work. The five are the simplest, easiest and most broadly useful exercises I have developed (my books and videos describe many more). The exercises are concrete, specific, and reliable. They are not philosophy. They are physiology.
They are simple enough that people can learn them easily and even teach them to others right away. Applying the exercises in conflict resolution and peacemaking is simple enough that people can use them effectively right away.
MOVEMENT RIDDLES
As a preparation for the five exercises, I use the following movement riddles to grab people’s attention and get across some key concepts. I have a student stand in a strong forward-stride stance, and I explain that I want him to resist me when I push on his shoulders. I ask whether the person has any physical or psychological issues which would make that unsafe. I ask him to lean into me a bit and make it very hard for me to move him. The demonstration is much more startling when I work with somebody much bigger and stronger than I. Then I ask the client to raise his eyebrows, and immediately I can easily push him toward his rear. Why? The answer is very simple. Raising the eyebrows is part of the fear/startle reflex, and another part is leaning back to get away from the object of fear. When one part of the startle response is done in the body, the rest of the response fires off too – even though there’s nothing to be afraid of.
following movement riddles to grab people’s attention and get across some key concepts. I have a student stand in a strong forward-stride stance, and I explain that I want him to resist me when I push on his shoulders. I ask whether the person has any physical or psychological issues which would make that unsafe. I ask him to lean into me a bit and make it very hard for me to move him. The demonstration is much more startling when I work with somebody much bigger and stronger than I. Then I ask the client to raise his eyebrows, and immediately I can easily push him toward his rear. Why? The answer is very simple. Raising the eyebrows is part of the fear/startle reflex, and another part is leaning back to get away from the object of fear. When one part of the startle response is done in the body, the rest of the response fires off too – even though there’s nothing to be afraid of.
Another riddle: The student stands in the same stance as before, resisting my push on his shoulders. This time I have the person say something friendly to me and note what happens in his body. Usually there is no effect. Then I have him say something unfriendly and insulting. Almost always the immediate effect of saying something negative is that I can push him back fairly easily. Why? The body responds to unfriendliness and unkindness by contracting, and that interferes with fluid use of the body to achieve effective balance and movement.
A third riddle: Many people use anger as a source of power. Push on the student’s shoulders as in the second riddle. But this time have the student think of something that makes him angry. See whether that creates more stability and strength or less. Most people will experience less balance and less strength when they are angry as compared to when they are calm and kind.
A fourth riddle: Stand in front of a student and grasp his wrist. Now pull him toward you. The student’s task is to not be pulled toward you. Most people brace their posture and resist the pull. That is, of course, one strategy for succeeding at doing what was asked for. However, that strategy, though effective, takes a lot of hard work. I suggest that they simply walk forward. People realize that they understood the instruction to mean “Don’t move forward.” However , the instruction actually was to not be PULLED forward, and the easiest way to do this is to walk forward—and take over the movement. This riddle is about taking a different perspective and how that opens up new options for dealing with difficult situations.
I have found a number of somatic riddles, and they all hinge on taking a different perspective in some fashion. The point is that the body is where peace can be observed and practiced in a clear and concrete way, if you have the tools. These three riddles point to the fact mind and body are the same thing. And they also point to the fact that the optimal way of functioning is based on the integration of power and love.
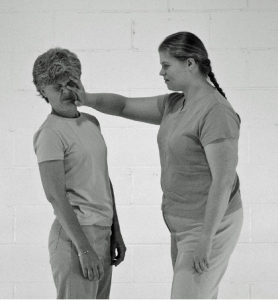
DISTRESS RESPONSE
Emotions are physical actions in the body. Feelings are what those actions “taste” like to the person who is doing them.When we are threatened or challenged or hurt, we contract or collapse our posture, breathing, and attention— as the picture of the woman being touched shows. That is the distress response, and it is usually experienced as feelings such as fear, anger, helplessness or numbness.
These powerful physical responses hijack the rational mind and compassionate heart and move our thinking and acting toward oppositional and violent ways of dealing with the challenges we face. Being hurt or hurting someone often leads to dehumanization of the other person and of oneself too, and out of this comes more prejudice and more distress.
When the distress response gets locked into the body, that is the trauma state. You should be aware that in any group of 25 people or so, there are likely to be 1 or 2 survivors of child abuse or other trauma, and body awareness exercises sometimes can throw people into painful emotional states that they had been suppressing. These five peacemaking exercises are also effective for empowerment in trauma recovery work. However, working with trauma is more delicate and requires broader skills and understanding. If someone drops into trauma recall as you teach embodied peacemaking, keep breathing and stay relaxed and steady, and you will find a way to steady the person. Then refer them to a qualified professional.
FIVE EXERCISES
Just as you cannot dig a hole in the water, you cannot stop doing a particular behavior. Instead, you have to start doing an incompatible and more useful behavior. The opposite of and antidote to the physical state of smallness is a state of centered expansiveness. This state of calm alertness and compassionate power moves our thinking and acting toward empathic, assertive and peaceful ways of handling conflicts. And living in the present with compassionate power breaks the chains that bind people to their past trauma.
RELAXED CORE: Let your tongue hang softly in your mouth. Most people will feel that this relaxes the muscles around the neck and shoulders.
Let your shoulders and your armpits hang loose and notice the effect on the rest of your body. Let your belly plop loose. Let your legs hang on the ground. When you breathe, where is the movement in your body? Up into your chest perhaps? That is fear/startle breathing. As you inhale, let your belly expand. Your chest should also expand as you inhale, and the focus of the breathing movement will be on relaxing/expanding the belly. Most people find this very calming.
SMILING HEART: Everyone has something or someone that makes them happy inside —perhaps a friend, a child, a flower, a piece of music. Stand with your eyes closed, and spend a moment thinking about whatever it is that makes you smile inside. What hap-
pens in your body? Most people experience a softening and warmth in their chest, and a freeing up in their entire body.
Can you use your image while you are in a conflict to keep your body stabilized in the feeling of compassion? That would alter your relationship to your opponent. Can you stay anchored in this feeling even when thinking about difficulties in your life?
SHINING: Imagine that you are a star or a firefly or a light bulb. What do you do? You shine. Feel every inch (or centimeter) of your skin glowing outward, as you shine in every direction—as far out as you wish. How does that feel? Most people experience this as spacious and calm.
Some people find it easier to imagine something tangible to reach their awareness toward. A popular image is that of reaching toward  slices of pizza.
slices of pizza.
 POWER SITTING: Power is necessary to allow
POWER SITTING: Power is necessary to allow
us to function in a loving and peaceful manner. Love without power is weak and ineffective. And of course power without love is brutal and destructive. The development of power starts with postural stability.
Stand in front of a chair, and get ready to sit down – but in a new way. With each hand, touch your hip joints. Not the hip bones – which are the top edge of the pelvis, but the hip joints – which are in the fold where the legs bend. Imagining a line from the hip joints to the tailbone, push your tailbone back and down along that line. This will lean your torso forward, but not too much. It will take you down to a sitting position. This way of sitting down creates a posture that is very strong yet without effort (see the photo). Most people feel calm, alert, and dignified in this posture.



POWER WALKING: There is a standing equivalent of the sitting posture. Walk around barefoot, pay attention to how your legs and feet make your body move forward across the floor. Many people swing a leg forward, and the weight of the leg drags their body forward. Some people put a foot on the floor out in front of them and then pull themselves forward with it. Some people feel that when their foot is behind them, they push themselves forward with it. Stand with your feet together, and jump up in the air. To jump up, you push down. To walk forward most efficiently, you push to the rear with the back leg. A simple way to experience this is to have a partner grasp your belt from behind you. Your partner should pull back and offer moderate resistance to your walking. You will experience that the only way to move forward is to push backwards with the rear leg. People generally experience that when they walk with this awareness of the down/back thrust of the feet, their walk becomes more erect, clearer and more energetic. It is mechanically more efficient and powerful, and it is also much more psychologically confident and alert.
APPLICATIONS
How would you use this body awareness process in managing a conflict? Identifying the emotions as body actions, you could ask, “Where in my body am I doing something? And what am I doing there?” And once you identify what and where the emotions are, you can manage them and break their hold on you. It will not itself be the solution to the conflict, but it will enable you to think and act more freely and come up with a solution if one is possible.
Body-based self-regulation (Embodied Peacemaking) enables people to control their fear and anger and act in peaceful, healthy ways. Deliberately widening and opening yourself in the midst of conflict allows a cooperative peace process to begin unfolding. If you stay centered, you will not see the other person as an enemy or feel the urge to hurt him/her. Deliberately opening when you want to contract or collapse weakens the physical habits within you and lets you live in a centered strong civilized place. Even though this process often works for people right away, regular practice of somatic centering will make it easier to stay centered when a conflict arises.
If the conflict involves a physical attack, though it is counterintuitive, being kind and generous will free your body so that you can fight more effectively – if fighting is the only choice. In the usual verbal disputes, body-based self-regulation enables people to stay focused on the substance of the dispute and not get distracted by the emotions that are stirred up by the dispute. Beyond that, if you notice that your emotions are hijacking the dispute and preventing calm, respectful dialoging, you could ask for a 5-minute body awareness and breathing break.
THROWING TISSUES: A PRACTICE ATTACK
How can we get a practical handle on what conflict is and what its physical effects are? What we need to begin the investigation is a small piece of violence. If it is safe and small-scale, it will not cause unbearable stress, and it will be safe enough to
study. But it must be real enough to arouse a response in you, or it will be not be worth studying.
Ask your partner to stand about six or eight feet away (about two meters) from you and throw balled up tissues at you. Most people find that this mostly symbolic gesture does arouse some fear, but since the “attack” is minimal, so is the fear.
Calibration is important. The exercise must be matched to the student. In working with people who don’t feel much, it is often necessary to increase the stimulus intensity so that they get a response large enough for them to notice. I might wet the tissue so it hits with a soggy and palpable thud. Or I might throw pillows instead of tissues.
On the other hand, I often have people tell me that even throwing a tissue at them feels too intrusive and violent. In that case, standing back farther so that the tissue doesn’t reach them, makes the “attack” even more minimal. Or it may be necessary to do just the movement of throwing the tissue without a tissue at all. Perhaps turning around and throwing the tissue in the wrong direction will help. Or just talking about throwing a tissue, but not moving to do so at all.
The point is to adjust the intensity of the “violence” in this exercise so that it is tolerable and safe for you to examine. For most people that means revising the attack downward in intensity.
Once you have chosen your preferred attack, have your partner attack you and notice what happens in response to the attack. What do you feel? What do you do? What do you want to do?
There are a number of common reactions to the attack with the tissue. People being hit often experience surprise or fear. They may feel invaded and invalidated. Frequently they tense themselves to resist the strike and the feelings it produces. Some people giggle uncontrollably or treat the attack as a game. Many people get angry and wish to hit back. People may freeze in panic, and some people go into a state of shock or dissociation.
Most people talk about feelings and mental states. They are surprised, angry, afraid and so on. They want to escape or fight back. However, a very different way of paying attention to yourself is possible. Notice the details of your muscle tone, breathing, body alignment, and the rhythms and qualities of movement. Where in your body do you feel significant changes? What are you feeling in those locations? Rather than speaking in mental terms— about feelings, thoughts and emotions—it can be very productive to speak in body- based language.
By paying attention to the physical details of your responses, you will begin to see more deeply into the ways you handle conflict. And learning to notice what you do is the first step in changing and improving what you do. Notice what you do in your throat, belly and pelvis. What happens in your chest and back? Notice what you do in your face and head. Notice what you do with your arms/hands and legs/feet. What happens to your breathing? Is there anything else to pay attention to?
Most people realize that they tighten up when they are attacked. They may clench their shoulders or harden their chests. They most likely tense or stop their breathing. They may lean back or lean forward, but it is a tense movement. Sometimes this tension is fear, and people shrink away from the attack. Sometimes this tension is anger, and people lean forward and wish to hit back. Do you do any of these things? Do you also do something else? Many people find that they get limp as a response to being hit. Their breathing
and muscles sag; or they look away and space out, simply waiting for the hitting to be over. They may feel their awareness shrink down to a point or slide away into the distance. Many people find that they experience both rigidity and limpness simultaneously in different areas of the body.
Some people find the role of the attacker far more difficult than the role of the victim, but we will focus on the responses of the person being attacked. However, one idea might make the attacker role easier for you. It will help to remember that your attack is a gift to your partner. By being concerned and benevolent enough to attack your partner, you are allowing them the opportunity to develop self-awareness skills. Without your gracious cooperation, they would not be able to learn these skills, and when they faced real challenges in their lives they would be completely unprepared.
The common denominator in responses of tensing or getting limp is the process of getting smaller. Fear and anger narrow us physically, mentally, emotionally, and spiritually. However, softening and opening the body is the antidote to contraction or collapse.
FURTHER PRACTICE
How can you go further in learning and using Embodied Peacemaking? Daily practice of the for exercises described here will take you a long way.
You could also work through the exercises in one or another of my books or videos, which are available on my website. You could form a study group to have partners to practice with. Unfortunately life brings many conflicts and many traumas, so
there will be no shortage of opportunities for practice.
PAUL LINDEN, Ph.D. is a somatic educator, a martial artist, and an author. He is the developer of Being In Movement® mindbody education. He has a B.A. in Philosophy and a Ph.D. in Physical Education, and is an authorized instructor of the Feldenkrais Method® of somatic education. He has been practicing and teaching Aikido since 1969 and holds a sixth degree black belt in Aikido as well as a first degree black belt in Karate. His work involves the application of body and movement awareness education to such topics as stress management, conflict resolution, computer ergonomics, music or sports performance, and trauma recovery.
Some of Paul Linden’s books and videos
Embodied Peacemaking —Five Easy Exercises. 8 page handout. Free download.
Reach Out: Body Awareness Training for Peacemaking—Five Easy Lessons. 46 pages.
Free download.
Embodied Peacemaking: Body Awareness, Self-Regulation and Conflict Resolution. 164
pages.
Teaching Children Embodied Peacemaking: Body Awareness, Self-Regulation & Conflict
Resolution. 70 pages
Feeling Aikido: Body Awareness Training as a Foundation for Aikido Practice. 300 pages.
Winning is Healing: Body Awareness and Empowerment for Abuse Survivors. 410 pages.
Embodying Power and Love: Body Awareness & Self-Regulation. 10 hour video
Talking with the Body: Body Awareness Methods for Professionals. 9 hour video
Downloadable from www.being-in-movement.com
Paul Linden, PhD
www.being-in-movement.com
paullinden@aol.com
How can people bear to cause other people pain? How can people embrace racism, sexism, political and religious violence, and hatred? A major part of the answer is that it is all too easy for people to see the world through fear and anger and to view other people as not fully human. But in dehumanizing others, people dehumanize themselves. And in so doing, they become numb and can hurt others without feeling it.
However, this is not simply a political, cultural, psychological or spiritual problem. This whole process takes place in the body. Though most people do not notice it, emotions are actions that we do in the body. Hatred is something that is done in the body.
To change how we feel, it is not enough just to decide to stop destructive feelings. The body must be taught to not hate. And in a sense that is impossible. It is impossible to stop a negative. It must be replaced with a positive. Through specific and concrete body techniques, it is possible to teach people to create, understand and use in their lives a body state of awareness, power and compassion. This is not the whole solution, but it is a necessary foundation. It moves people to feel others as human and to care what happens to them.
Based on his 50 years of practice, Paul has developed a short series of simple, powerful transformational exercises. By using concrete and testable language in teaching, Paul can help people learn very rapidly how to apply these techniques effectively in their lives.
PAUL LINDEN, PhD is a body awareness educator, a martial artist, and an author. He is the developer of Being In Movement® mindbody education, and founder of the Columbus Center for Movement Studies in Columbus, Ohio. He holds a BA in Philosophy and a PhD in Physical Education. He has been practicing and teaching Aikido since 1969 and holds a sixth degree black belt in Aikido as well as a first degree black belt in Karate. In addition, he is an instructor of the Feldenkrais Method® of somatic education. He has extensive experience teaching people such as musicians, athletes, business people, computer users, pregnant women, adult survivors of child abuse, and children with attention deficit disorder. Paul has written numerous papers on diverse topics. He has also authored a number of e-books and videos, among which are (at www.being-in-movement.com):
• Embodied Peacemaking: Body Awareness, Self-Regulation and Conflict Resolution
• Winning is Healing: Body Awareness and Empowerment for Abuse Survivors
• Embodying Power and Love: Body Awareness & Self-Regulation (10 hour video)
• Talking with the Body: Training for Helping Professionals. (10 hour video)